Living Well With cGHVD
Chronic graft-versus-host disease (cGVHD) can deeply affect daily life because it is a long-lasting condition that may involve many parts of the body and often requires ongoing treatment. It develops in about 30% to 70% of the people who receive an allogeneic (donor) stem cell transplant. Even though cGVHD is driven by similar immune changes in the body, each person’s experience can be very different. Some people may have mild symptoms, while others face more serious complications that affect their independence, comfort, and emotional well-being.1
Many people with cGVHD notice changes in their physical strength, energy, and ability to carry out daily activities. Joint stiffness, skin tightening, fatigue, dry eyes or mouth, breathing problems, and digestive symptoms can all interfere with a person’s work, exercise, and social life. For some, returning to work or normal routines may take much longer than expected, and others may need to adjust their lifestyle permanently.1
Beyond physical symptoms, cGVHD can also affect a person’s emotional and mental health.1
Many patients describe the challenge of adapting to new restrictions in their everyday lives, especially when symptoms change over time or flare unexpectedly.1
Support networks
For patients navigating cGVHD, multiple specialized support networks offer peer connections, professional counseling, educational resources, and practical assistance. These organizations address the unique physical, emotional, and financial challenges that cGVHD presents.
Supportive care
Supportive care is an essential part of living with cGVHD. It is available to everyone with cGVHD, at any stage of the disease—not just at the end of life. Supportive care focuses on helping you feel as well as possible by preventing and managing symptoms, reducing treatment side effects, and supporting your physical, emotional, and practical needs. You may also hear this called palliative care. It can be provided alongside your cGVHD treatment.2
Because cGVHD and its treatments affect the immune system and many organs, supportive care plays a major role in maintaining your day-to-day comfort, energy, and independence. Many people receiving treatment for cGVHD need support for symptoms such as diarrhea, fatigue, nausea, pain, appetite changes, and emotional distress.2
Supportive care can help you:
Manage symptoms and treatment side effects
Coordinate your care across different specialists
Make informed treatment decisions
Plan for future medical care
Improve overall comfort and daily functioning
Preventing and treating infections
People with cGVHD often have a weakened immune system, which increases the risk of serious infections. Infections may be caused by bacteria, viruses, or fungi, and some can become life-threatening if not treated early.2
Your care team may prescribe antibiotics, antifungal medications, or antiviral drugs to treat infections or prevent them from developing. For example, azithromycin (Zithromax or Z-Pak) may be used to help treat lung problems related to cGVHD. It is important to take all medications exactly as prescribed and to contact your care team right away if you develop fever, cough, chills, or other signs of infection.2
Managing digestive symptoms and nutrition
Diarrhea is common in cGVHD and can be frequent and uncomfortable. Your care team will give you guidance on how to manage it and may prescribe medications to slow bowel movements. Over-the-counter medicines may help, but you should always check with your provider before using them. Drinking plenty of fluids is essential to prevent dehydration. Let your care team know immediately if you see blood in your stool.2
Some side effects of cGVHD or its treatments can cause poor appetite, nausea, vomiting, mouth sores, or stomach upset. Healthy nutrition is especially important during treatment. A registered dietitian can help you choose foods that are easier to eat and meet your nutritional needs. If you are losing weight or struggling to eat, your care team can offer medications and practical strategies to help.2
Fatigue, pain, and physical comfort
Fatigue is 1 of the most common and frustrating symptoms of cGVHD. It may be caused by inflammation, low blood counts, medications, or poor sleep. Various treatments can help, including medication adjustments, physical activity programs, and nutrition support. Let your team know how tired you feel and how it affects your daily life.2
Pain is also common and may come from joint stiffness, muscle involvement, eye irritation, mouth sores, or abdominal cramping. Your care team can recommend pain-relief strategies or refer you to a pain or palliative care specialist for additional support. Managing pain effectively is a key part of improving quality of life.2
Emotional health and distress
Living with cGVHD can be emotionally overwhelming. Many patients experience distress, which may include feelings of sadness, fear, anger, guilt, or helplessness. Anxiety, depression, and sleep problems are also common during long-term illness.2
It is important to talk openly with your healthcare providers about how you are feeling emotionally, not only physically.2

You are not alone in this journey, and support is available for both you and your family.
Nausea and vomiting
Nausea and vomiting can be signs of cGVHD or side effects of treatment. Medications are often used to control these symptoms and help you continue eating and drinking. Always let your care team know if nausea is affecting your ability to take medications, eat, or stay hydrated.2
Being an advocate for yourself in cGVHD care
You play a critical role in your own supportive care. Being an advocate for yourself means speaking up about your symptoms, concerns, and goals so your care team can respond quickly and effectively.2,3
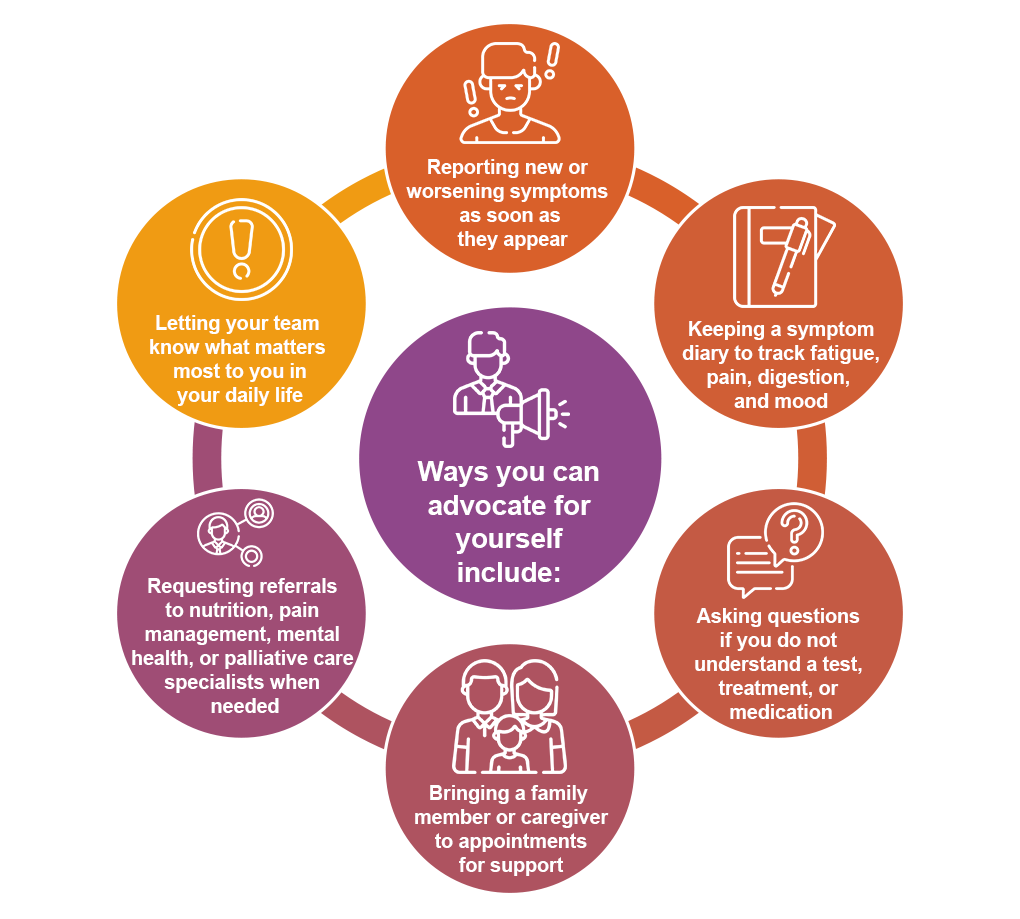
Your voice helps guide your treatment plan and ensures that care is focused not only on controlling the disease, but also on protecting your comfort, independence, and quality of life.
References
- Williams E, Skinner L, Hudson R, et al. A vignette study to derive health-related quality-of-life weights for individuals with steroid refractory chronic graft-versus-host disease receiving third-line therapy in the United Kingdom. J Health Econ Outcomes Res. 2025;12(1):58-65. https://doi.org/10.36469/001c.125546
- National Comprehensive Cancer Network (NCCN). Graft-versus-host disease. 2025. https://www.nccn.org/guidelines/guidelines-detail?category=patients&id=63. Accessed 12/14/2025.
- National Comprehensive Cancer Network (NCCN). Hematopoietic cell transplantation. Version 2.2025. https://www.nccn.org/guidelines/guidelines-detail?category=3&id=1501 Accessed 12/14/2025.