Individualizing Care in cGVHD
Chronic graft-versus-host disease (cGVHD) affects multiple organs, changes over time, and often requires long-term immunosuppression. Because of this complexity, care must be individualized and attention given to balance infection prevention, organ-specific monitoring, and coordinated support from a multidisciplinary team (MDT).1
Patient support and infection prevention
Infection remains the leading cause of death in patients with cGVHD, especially as immunosuppression is intensified. Prevention and early detection should be part of every visit.1
For antimicrobial prophylaxis and viral surveillance, provide antimicrobial prophylaxis in line with cancer-related infection guidelines when systemic immunosuppression is started or escalated. Monitor for cytomegalovirus (CMV) reactivation, which carries substantial morbidity and mortality in allogeneic hematopoietic cell transplant (HCT) recipients.1
Avoid live vaccines in all patients with active GVHD or those on significant immunosuppression. Ensure revaccination for coronavirus disease 2019 (COVID-19) and other inactivated vaccines per posttransplant schedules, recognizing that responses may be blunted early after HCT.1
IVIG and special situations1
Routine use of prophylactic intravenous immunoglobulin (IVIG) is not recommended for most patients with cGVHD. It may be considered when:
- Umbilical cord blood (UCB) transplant recipients have significant hypogammaglobulinemia
- Children undergo transplant for inherited or acquired B-cell deficiencies
- Patients with cGVHD experience recurrent sinopulmonary infections despite standard prophylaxis
Managing steroid-related risks
High-dose or prolonged corticosteroid therapy in cGVHD significantly increases the risk of infectious, metabolic, and skeletal complications and therefore requires proactive risk mitigation. Clinicians should recognize the strong association between high-dose steroids and viral, bacterial, and fungal infections, as well as glucose intolerance and adrenal suppression. All patients receiving high-dose corticosteroids should receive routine vitamin D and calcium supplementation, and dual-energy X-ray absorptiometry (DEXA) scanning should be recommended for those with current or prior high-dose steroid exposure or additional osteoporosis risk factors. Ongoing screening for steroid-related myopathy, mood disturbances, and weight gain is essential, with early involvement of endocrinology or bone health specialists when clinically indicated.1
Patient support strategies
Patient support strategies are a critical component of cGVHD management and should actively engage both patients and caregivers in ongoing monitoring. Patients and caregivers should be encouraged to maintain a detailed symptom diary to track key warning signs such as fever, cough, diarrhea, new or worsening pain, oral sores, and vision changes, which can facilitate earlier recognition of disease flares or treatment-related adverse events. For patients who live far from transplant centers, telehealth visits can be effectively used to maintain close clinical contact and continuity of care; however, clinicians should emphasize the continued importance of periodic in-person evaluations for comprehensive physical examination and organ-specific assessment.2
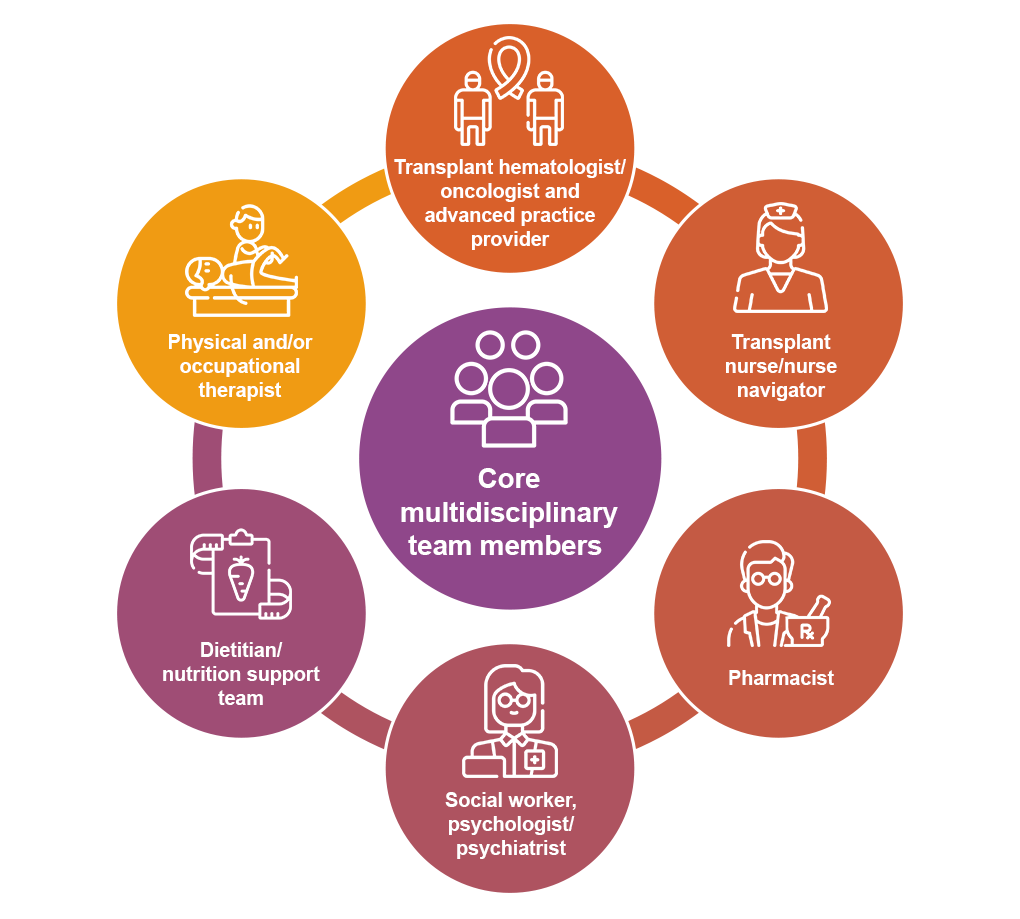
Multidisciplinary care: Who’s on the team?
The transplant team should remain the central point of contact, coordinating referrals and ensuring that all specialists understand the unique needs of allogeneic HCT survivors.3,4
Organ- and symptom-driven referrals
Depending on organ involvement and patient-reported symptoms, additional specialists may include:
- Dermatology: Skin rash, sclerotic changes, high skin-cancer risk
- Dentistry/oral medicine/ears, nose, and throat (ENT) specialty: Oral cGVHD, mucosal lesions, dental decay
- Ophthalmology: Ocular dryness, pain, photophobia, visual changes
- Gastroenterology/hepatology: Chronic diarrhea, malabsorption, liver test abnormalities
- Gynecology: Vulvovaginal dryness, dyspareunia, dysuria, scarring/stenosis
- Urology: Genital or urinary sclerosis, phimosis, urethral symptoms
- Pulmonology: Cough, dyspnea, declining PFTs, suspicion for bronchiolitis obliterans syndrome (BOS)
- Neurology/physiatry: Neuropathy, myopathy, gait disturbance
- Cardiology: History of arrhythmias or cardiovascular disease, particularly when BTK inhibitors such as ibrutinib are used
Close bidirectional communication between specialists and the transplant center is essential so that changes in therapy (eg, immunosuppression, anticoagulation) are visible to all.
Organ-specific monitoring tips1,2
Routine, structured assessments starting around Day 100+ and continuing every 1 to 3 months—then spaced out as immunosuppression tapers—help catch problems early.
Oral cGVHD
Patients with oral involvement should be monitored for:
- Xerostomia (dry mouth): Ask about difficulty swallowing dry foods, need for constant fluids, altered taste
- Oral squamous cell carcinoma (SCC): Look for nonhealing ulcers, indurated plaques, leukoplakia, or erythroplakia; refer promptly for biopsy
- Oral thrush: White plaques, burning, angular cheilitis; treat promptly and reassess for inhaled or systemic steroid exposures
Supportive and preventive strategies include baseline and 6- to 12-month dental and oral medicine exams for all patients with cGVHD, along with daily fluoride, saliva substitutes, sugar-free gum, and meticulous oral hygiene. Educate patients to report new mouth pain, color changes, or difficulty opening the mouth between visits.
Ocular cGVHD
Ask at each visit about dryness, foreign-body sensation, excessive tearing, light sensitivity, redness, or blurred vision. Arrange baseline and periodic ophthalmology exams, especially during the first posttransplant year or when symptoms arise. Management may include lubricating drops/ointments, punctal plugs, topical anti-inflammatories, and protective eyewear. Encourage patients not to ignore subtle changes—early ocular inflammation can progress quickly.
Gastrointestinal/nutritional involvement
In patients with gut cGVHD, monitor for diarrhea, weight loss, abdominal pain, and early satiety. Prolonged diarrhea warrants a workup for malabsorption (stool studies, nutritional lab tests, endoscopy as indicated). Because GI involvement increases the risk of malnutrition, involve a dietitian for caloric and protein optimization, vitamin/mineral replacement, and practical meal planning.
Hepatic involvement
Follow bilirubin, AST, ALT, and alkaline phosphatase periodically. Hydrophobic bile acid therapy such as ursodiol may be used to prevent or manage certain hepatic complications (per center practice). Educate patients about symptoms of liver dysfunction (jaundice, pruritus, dark urine).
Vulvovaginal and genital cGVHD
Common symptoms: Dryness, tenderness, dysuria, dyspareunia, bleeding, or tightness. All patients with vulvovaginal symptoms should be assessed by a gynecologist familiar with cGVHD. For men and women, genitourinary symptoms or sclerotic changes (eg, phimosis, urethral narrowing, scarring) warrant referral to urology and/or dermatology. Counseling about sexual health, lubrication, pelvic floor therapy, and dilator use can improve quality of life.
Pulmonary involvement
Obtain baseline PFTs pre-HCT and at Day 100+, 6, 9, and 12 months, then at least annually; more frequently in those with cGVHD. A ≥10% decline in forced expiratory volume in 1 second (FEV1) from baseline should prompt repeat testing and evaluation for BOS or other lung disease. Patients with respiratory viral infections plus forced expiratory volume in 1 second (FEV1) decline are at high risk and should be followed closely. Consider home spirometry or telehealth-assisted symptom checks for patients living far from PFT facilities.
Musculoskeletal/neurologic involvement
At each visit, assess range of motion using P-ROM, new stiffness, muscle cramps, limb swelling, or neuropathic symptoms. Early referral to physical and/or occupational therapy can help maintain function, prevent contractures, and support safe exercise.
Engaging patients as partners in ongoing monitoring2
Early recognition of cGVHD remains challenging despite standardized NIH criteria, which are variably applied in routine practice and often identify disease only after significant, potentially irreversible organ damage has occurred. Improved clinical implementation and discovery of earlier diagnostic markers to enable preemptive intervention is needed. The NIH published the Clinical Implementation and Early Diagnosis Working Group Report to provide early diagnostic tools to implement earlier diagnosis of cGVHD. Recommendations include:
- Provide education at key milestones (around Day 100+, during immunosuppression taper, at transfer back to community oncology or primary care)
- Teach patients to recognize sentinel symptoms—new rash, dry eyes, mouth sores, cough, dyspnea, genital discomfort, or functional decline—and to contact the transplant team promptly
- Consider structured symptom tools or apps (checklists, diaries, electronic patient-reported outcomes [PROs]) when feasible, while being sensitive to varying levels of health literacy
- Use telemedicine to extend expertise to community providers and to keep remote patients connected to the transplant center, always pairing virtual visits with periodic in-person exams
Individualizing care in cGVHD means more than choosing the right systemic therapy. It requires aggressive infection prevention, organ-targeted monitoring, and active patient participation. With this proactive, team-based approach, clinicians can better prevent irreversible organ damage, reduce treatment-related harm, and support long-term health and quality of life for survivors of allogeneic HCT.
References
National Comprehensive Cancer Network (NCCN). Hematopoietic cell transplantation. Version 2.2025. https://www.nccn.org/professionals/physician_gls/pdf/hct.pdf. Accessed 12/13/2025.
Kitko CL, Pidala J, Schoemans HM, et al. National Institutes of Health Consensus Development Project on criteria for clinical trials in chronic graft-versus-host disease: IIa. The 2020 Clinical Implementation and Early Diagnosis Working Group Report. Transplant Cell Ther. 2021;27(7):545-557. https://doi.org/10.1016/j.jtct.2021.03.033
GVHDnow website. First year after transplant: what should I be aware of? https://www.gvhdnow.com/stem-cell-transplant-journey/stem-cell-transplant-recovery Accessed 12/13/2025.
House Medicine website. The role of multidisciplinary teams in transplant success. https://housemedicine.com/the-role-of-multidisciplinary-teams-in-transplant-success/. Accessed 12/13/2025.